cardiac testing
Stress Test
A stress test is the principal non-invasive method for determining whether there are significant blockages in your heart arteries. However, many patients are confused or misled by the term “stress”—they wrongly assume it means that something bad is being done to the heart. In fact, all that term means is that the heart is asked to simulate a modest degree of exercise. In some patients this means ACTUAL exercise by walking briskly on a treadmill for a few minutes (no-one will ask you to run a marathon!)

In other patients who cannot walk on a treadmill (the elderly or those with physical injuries) the “exercise” is done for you by administration of a very short acting medication that reproduces the physiology of exercise, even with the patient still seated and at rest. The patient’s blood pressure, heart rate and continuous ECG are monitored carefully during the test. Patients are always in control and may stop the test if they feel uncomfortable. However, for most people the process is smooth and uneventful.
Stress testing is usually paired with some sort of imaging study of the heart. Most commonly this is a nuclear imaging study, in which a short acting chemical is given by IV which travels through the blood stream to the heart. The nuclear camera can detect the presence of this chemical in the blood stream. By following the chemical as it flows through the arteries of the heart, it becomes obvious if that flow suddenly stops in the middle somewhere. In that case the patient is diagnosed with a blocked heart artery, which means risk for heart attack. Additional tests or procedures may be done in this case to confirm the diagnosis of coronary artery disease and treat the patient to reverse this blockage and prevent heart attack.
Echocardiogram
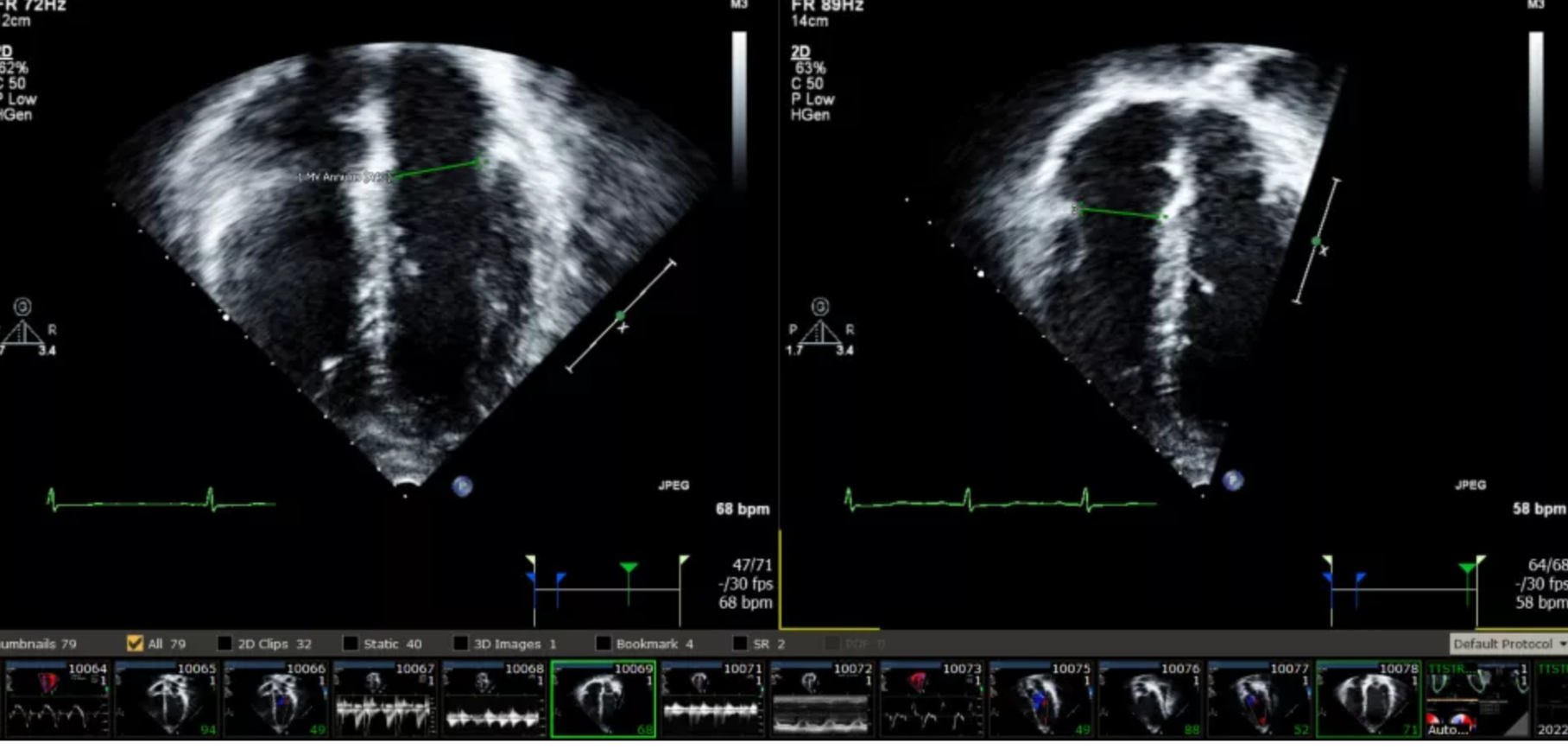
An echocardiogram, commonly known as an “echo,” is a type of test that uses sound waves to create pictures of your heart. It’s like the ultrasound that pregnant women get, but it’s for your heart. It produces a moving picture of your heart beating on a computer screen. These pictures show the size and shape of your heart, whether there are any areas of scar or damaged heart muscle, and how well your heart valves are working.
A common heart measurement made on every echo is an “ejection fraction” or EF—this one number provides an overall estimate of the strength of the heart muscle. The EF refers to the fraction of blood that is ejected from the heart with each heart-beat. In theory, if a heart were able to squeeze out all the blood in it’s chamber with each heart beat (which never happens) the EF would be 100%. If a heart doesn’t move at all, the EF is 0%. Normal patients have EFs in the range of 55-65%. An EF under 45% suggests damage to the heart muscle, with an EF under 35% being significant enough to be concerned about heart failure and cardiac arrest. On the other end of the spectrum, sometimes the opposite can happen—i.e. the EF can be too high, and suggest evidence of so-called “hypertrophic “ heart muscle disease, often from a familial genetic condition, or in response to the effects of longstanding hypertension (high blood pressure) on the heart. The EF is one of the measurements that is tracked over the course of multiple studies taken over several years in order to give an overall sense of the condition of the heart. Because an echo is non-invasive, painless and inexpensive, it is an ideal test to track the heart with.
Heart Monitor
A heart monitor, often referred to as a Holter monitor or cardiac event monitor, is a portable device that you wear to record your heart’s electrical activity over time. It’s similar to an EKG or ECG (electrocardiogram), but instead of taking a short snapshot of your heart at rest in a doctor’s office, a heart monitor tracks your heart rhythms over the course of a day or more, while you’re going about your usual activities or even while you’re sleeping.
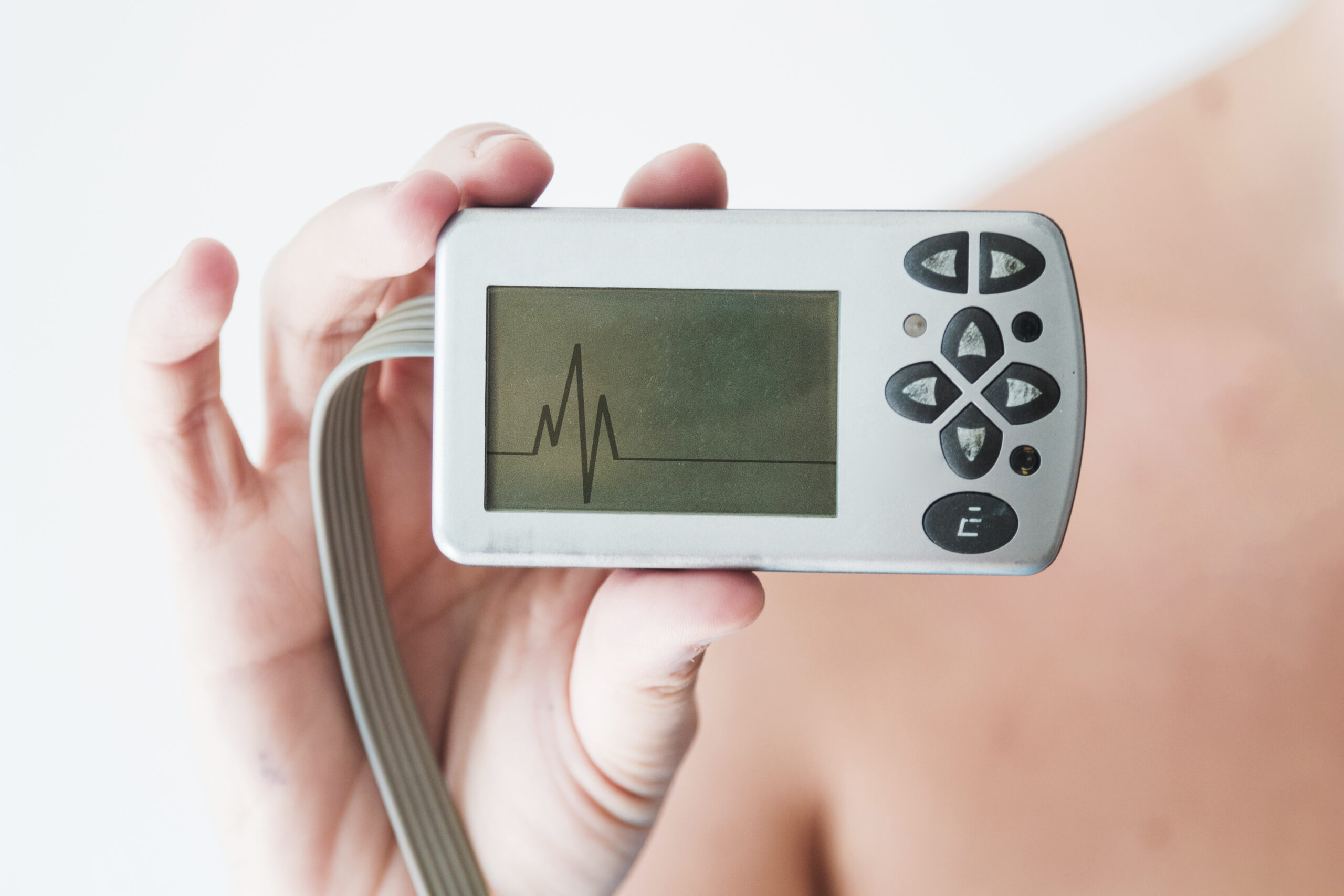
There are different types of heart monitors. A Holter monitor is typically worn for 24 to 48 hours and continuously records your heart’s activity during that time. An event monitor or MCOT monitor, on the other hand, is worn for several days and tracks a longer period of heart rhythm data. These types of heart monitors are preferred for arrhythmias that don’t happen every day, and require longer term monitoring.
These devices are small and lightweight. The monitor is usually about the size of a smartphone, and it connects to small, sticky patches (electrodes) that are attached to the skin on your chest. Some heart monitors have only 1 large patch instead of multiple small patches. And some heart monitors attach over wireless technology (Bluetooth) avoiding need for actual wires connecting between electrode and the recording device. Regardless of the specific type of heart monitor, all modern monitors are designed to be convenient to wear, and to remain hidden so that other people at work should not be aware you are wearing the device. The information from the heart monitor is collated and presented to the cardiologist for analysis.
There are many consumer devices on the market that claim to monitor heart rhythm through your watch or smartphone. While these devices can be useful in some situations, it is important not to confuse consumer electronics with medical grade equipment—and the medical service that supports medical equipment. No iwatch or iphone is a replacement for medical technology that is integrated in real time with a professional monitoring service, which is in turn communicating with the physician’s practice. You can buy an iwatch, but you cannot replicate that system. This is a common mistake in “techie” areas like Silicon Valley.
Electrocardiogram (ECG)
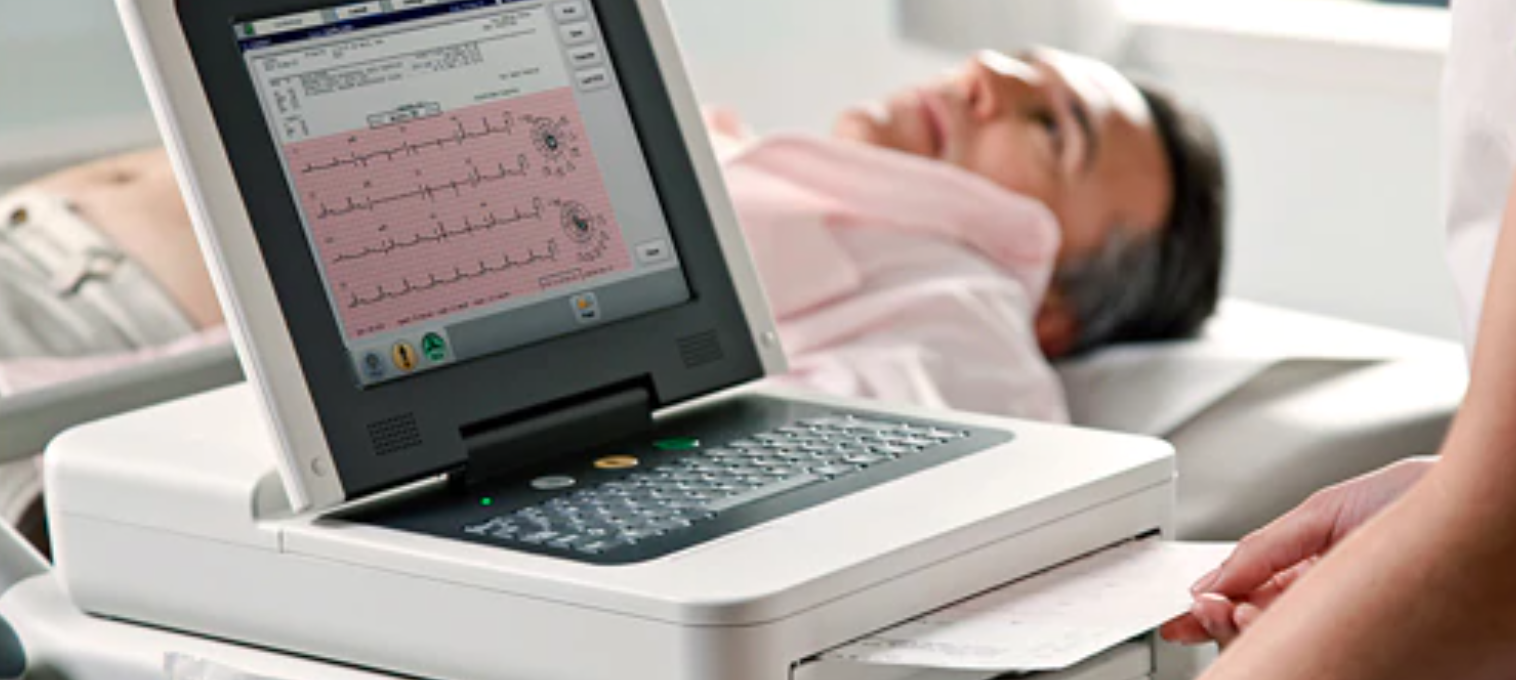
An electrocardiogram (ECG) is a simple, non-invasive test that provides important information about the electrical activity of your heart. It helps cardiologists evaluate the overall health of your heart and diagnose various heart conditions. During an ECG, electrodes (small, sticky patches) are placed on specific locations of your chest, arms, and legs. These electrodes are connected to an ECG machine that records the electrical signals produced by your heart.
The procedure for performing an ECG is straightforward and usually takes only a few minutes. You will be asked to lie down comfortably, and a healthcare professional will attach the electrodes to your skin using adhesive patches. The electrodes detect the electrical impulses generated by your heart as it beats, and these signals are transmitted to the ECG machine. The machine then produces a graph, known as an electrocardiogram, which displays the electrical activity of your heart in the form of waves.
The information provided by an ECG is valuable for cardiologists in assessing the overall health and function of your heart. The waves on the ECG graph represent different phases of the cardiac cycle, allowing the cardiologist to analyze the rhythm, rate, and regularity of your heartbeats. Abnormalities in the ECG waves can indicate various heart conditions such as arrhythmias (irregular heart rhythms), myocardial infarction (heart attack), ischemia (reduced blood flow to the heart), and abnormalities in the conduction system of the heart.
By studying the ECG results, your cardiologist can make educated guesses as to what is happening on the inside of your heart. However, it is important to realize that an ECG is a screening tool which is primarily useful because of how easy and inexpensive it is to acquire…..just a few minutes in your doctor’s office. It allows physicians to “get the ball rolling” in the right direction, but it is usually NOT the most accurate or definitive test that can be done to determine what is happening with the heart. For that, other imaging studies or procedures can be done to provide more accurate and detailed information about the heart.
