DEVICE IMPLANT
Pacemakers
Cardiac pacemakers and implantable cardioverter defibrillators (ICDs) are specialized devices designed to manage abnormal heart rhythms. Pacemakers are small devices implanted under the skin in the left upper chest region that regulate the heart’s rhythm by emitting tiny electrical impulses to encourage a regular heartbeat. An increase in the heart rate to “normal” ranges can lead to improved energy and activity level, and present symptoms of slow heart rate like dizziness, shortness of breath and fatigue.
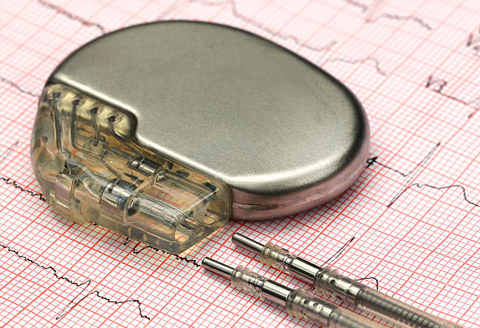
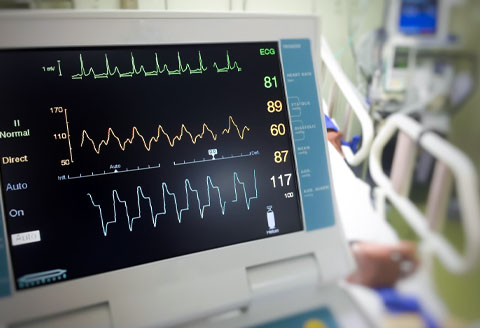
ICD
All ICDs are also fully functioning pacemakers. But in addition ICDs detect when the heart rhythm deteriorates into cardiac arrest (a very fast and chaotic heart rhythm) and can reverse this process urgently by delivering either rapid pacing pulses, or a life-saving electrical shock. These therapies terminate cardiac arrest and restore normal rhythm. Clinical studies show that in patients at high risk for cardiac arrest, ICD therapy is far superior to medical therapy at saving lives.
CRT
CRT, or Cardiac Resynchronization Therapy, is the term applied to the highest level of ICDs and pacemakers—called “bi-ventricular” ICDs and pacemakers. These devices have an additional pacing wire inserted close to the left lower heart chamber (left ventricle) which is the one primarily responsible for circulating blood throughout the body. This additional wire results in improved heart efficiency and can increase the strength of the heart beat. The device is primarily used in patients with symptoms of heart failure (shortness of breath, swelling) due to a damaged heart muscle, and in these patients often results in improvement in symptoms and cardiac function.
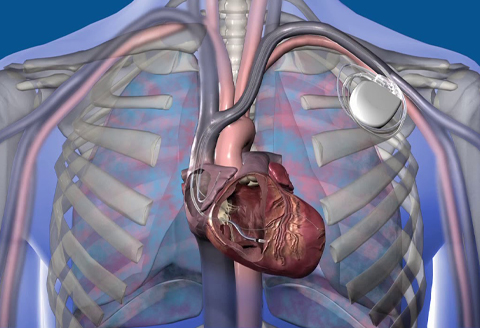
Dr Chow is an electrophysiologist with enormous experience and expertise in cardiac device implantation.

Device Remote Follow-up
According to Dr Chow, “Once the cardiac device goes in, the real work begins.”
The most difficult part of cardiac device treatment is not the implantation, but the follow-up. When patients leave the office and are at home, maintaining a focus on their device and arrhythmias is a challenge for any practice. At our practice, we have an established system of device follow-up that leverages technology such that we can periodically follow devices and arrhythmias even when the patient is at home. This remote device follow-up is combined with intermittent in-office device checks, and results in a high level of quality in follow-up for patients with cardiac devices. As an electrophysiology practice, the quality of our device follow-up process is at the highest level.
